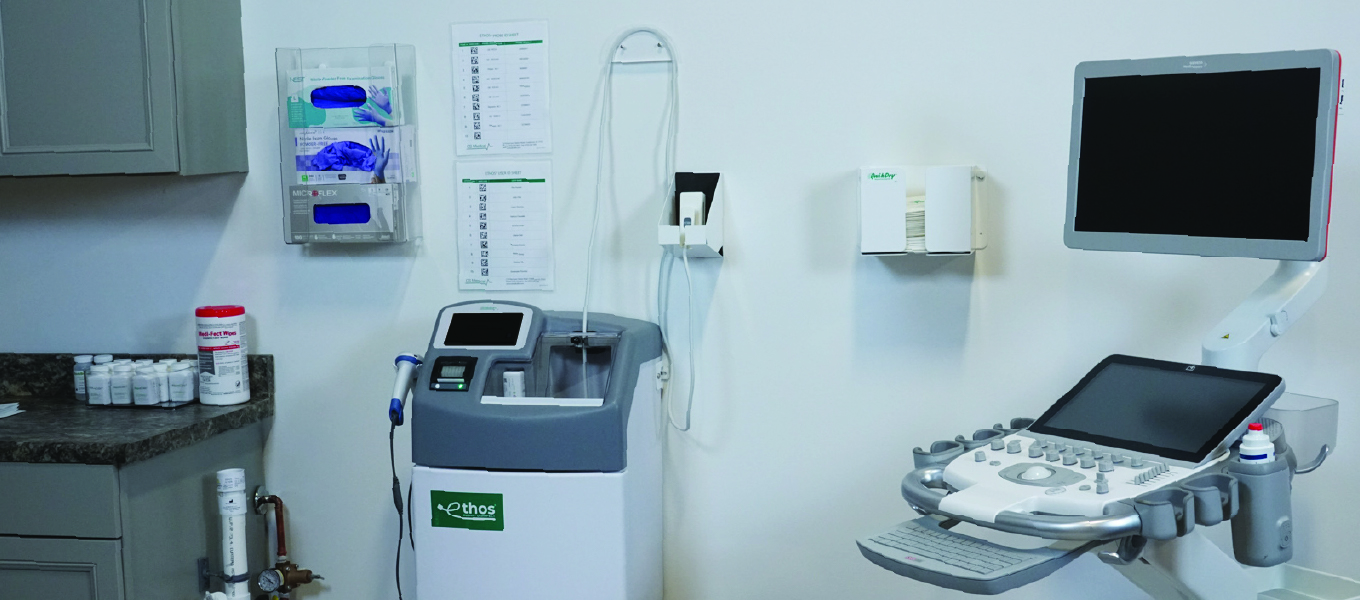
As you have been thinking about or reviewing existing SOP’s (Standard Operating Procedures), a key factor that is important to always remember is your staff and the complex job they are tasked to complete.
Staff involved in reprocessing and using ultrasound equipment should receive orientation training prior to commencing these responsibilities. Additionally, annual re-training should be performed for the duration of their employment. Training should establish the knowledge base required to safely perform reprocessing, safely use ultrasound in procedures with the goal of removing operator error, promote staff and patient safety and ultimately mitigate infection transmission risks. The Centers for Medicare and Medicaid Services Infection Control Worksheet requires surveyors to ensure the facility has documentation of training, competence and qualifications for staff involved in reprocessing.
Processing personnel should have documented competence in relevant cleaning methods, microbicidal processes, and equipment understanding related to the specific sterilization/HLD process used in the department. Furthermore, they should have knowledge of general sterilization or disinfection processes, infectious disease transmission principles, and aspects of liquid or chemical sterilization/HLD (if relevant), such as:
• Reprocessing
• Inspection of cleaning, drying and rinsing processes
• Monitoring of sterilization/HLD processes
• Maintaining documentation for traceability purposes
• Safety with regard to using the equipment and personal hygiene
• Use of PPE (where relevant) to protect skin, eyes, mucus membranes and clothing
Personnel that reprocess ultrasound probes are also required to participate in ongoing training programs which focus on orientation for their healthcare facilities and their departmental policies, infection prevention and control, use of reprocessing equipment, safety, attire, personal hygiene and compliance with local, state and federal regulations.
When establishing an equipment reprocessing policy, specifically for ultrasound probes, infection preventionists and other relevant subject matter experts should be involved when setting up the use of ultrasound probes for the first time; either when purchasing new ultrasound equipment or making changes to existing processes.
Considerations around safety:
The CDC guidelines and AAMI Standards both require staff and patient safety not be compromised by the chosen reprocessing workflows and processes.
Consider chemical exposure risks from bulk liquids and vapors:
Does the automated probe reprocessing system include a risk of disinfectant exposure, and if so has it been tested to be safe? Work area design considerations must be assessed (e.g.,
Cost:
The AAMI standards highlight cost-effectiveness factors that should be evaluated related to equipment (e.g., purchase, service and maintenance), consumables, PPE, energy, disposal costs and training).
Reprocessing time:
Consider time required to examine patients versus time for reprocessing. If there is high patient turnover it may be necessary to change the reprocessing procedure or purchase additional probes for effective turnaround time. Is this an opportunity to automate your probe reprocessing to give back time to the technician to accomplish other patient-centric tasks?
Reprocessing location:
If probes are reprocessed at point of use, then the disinfection method must be safe for patients and staff. The AAMI Standards and CDC Guidelines require a dirty to clean workflow during reprocessing. This should be observed regardless of the reprocessing location with designated dirty and clean areas to prevent cross contamination. If the transport of dirty or clean devices is required to a central reprocessing area, then a probe transportation protocol must be observed to prevent mixing of dirty and clean instruments. Is the transport method of the dirty or clean probe sufficient enough as to not promote probe damage or mix-up?
Automated or manual reprocessing:
Consideration should be given to automation versus manual processes. It is well accepted that automated processes minimize the influence of human factors on reprocessing outcomes and should be adopted where possible.
Ultimately, the staff member charged with developing, implementing and measuring what an effective reprocessing procedure is can be challenging and time consuming. The final standard operating procedure is one with many components but a primary focus should remain on the employee and how best to ensure staff competence that will ultimately reduce human errors.